Explore our world-class facilities, modern treatments, and compassionate care — setting new standards in taluk-level healthcare across the state.
Future services for advanced procedures like stenting, balloon angioplasty, and diagnostic catheterization for coronary artery disease.
Planned interventional unit for angiography, angioplasty, and device-based heart procedures under sterile and monitored conditions.
Visual and printed content to educate patients on heart health, disease prevention, medication adherence, and rehabilitation.
Skilled staff trained in cardiac care protocols, emergency response, ACLS, medication administration, and patient monitoring.
Coordination with tertiary hospitals for advanced cardiac interventions, surgeries, and electrophysiology studies as per patient need.
Post-dialysis observation zone with resting beds to monitor patients for fatigue, hypotension, or other complications after treatment.
Convenient availability of prescribed renal medications and diagnostic tests within hospital premises to support integrated kidney care.
Real-time imaging system to assess kidney size, stones, cysts, and post-biopsy complications at the nephrology department.
Certified staff trained in hemodialysis protocols, machine operation, patient handling, and emergency response during renal procedures.
Dedicated area or display offering leaflets, posters, and counseling on kidney disease prevention, dialysis care, and lifestyle management.
Digitized or manual recordkeeping of dialysis sessions, parameters, complications, and patient vitals for efficient care continuity and audits.
Designated sterile-ready area with provision to install ultrasound machine for nerve block procedures.
Color-coded emergency drug trays and wall-mounted dosage charts for rapid, error-free response during critical scenarios.
Organized storage for medications, syringes, circuits, and disposables ensuring easy access and stock maintenance.
Support staff trained in machine handling, drug preparation, and assisting anesthesiologists during procedures and emergencies.
Trained team and alert system for managing intraoperative complications or anesthesia-related emergencies swiftly.
Systematic record-keeping of pre-anesthesia evaluations, risk classifications, and consent forms for reference and legal compliance.
Essential hardware components, diagnostic kits, and tools for in-house repair and emergency response.
Software or physical tracking setup for maintaining stock, monitoring asset usage, and scheduling preventive maintenance.
Specialized instruments used to verify accuracy, safety, and functionality of biomedical devices during servicing and inspection.
Biomedical personnel trained in infection control, fire safety, biomedical waste handling, and regulatory compliance.
Organized contact system for quick access to vendors, suppliers, and OEMs for service, support, or parts replacement.
Established SOPs and kits to ensure technician and patient safety during electrical, mechanical, or biomedical emergencies.
Easy access to skin scraping tests, KOH mounts, and dermatology-related medications within the hospital ecosystem.
Color-coded bins, sharps containers, and biomedical waste protocols for safe disposal of skin procedure-related waste.
Accessible hand hygiene stations and disposal bins to support infection control and patient safety.
Collaboration with NLEP, PULARI, or health inspectors for referrals, awareness camps, and community-level dermatological support.
Nurses trained in topical application, patient prep, wound care, and dermatology OP flow management.
Environment conducive for respectful care and privacy across all genders, especially for STI or cosmetic consultations.
Organized documentation system for storing clinical notes, audiological test results, follow-ups, and treatment outcomes for continuity of care.
Established network for referring complex ENT surgical cases to tertiary care centers with advanced operative and postoperative facilities.
Connectivity to imaging and laboratory diagnostics for ENT-related investigations like X-rays, blood tests, CT scans, and thyroid panels.
Skilled nursing team familiar with ENT protocols, patient positioning, suctioning, post-procedure care, and counseling support.
Pamphlets, posters, and digital content to educate patients on ear care, allergy control, and voice hygiene.
Portable suction with sterile surgical tools for procedures like aural toileting, abscess drainage, or foreign body removal.
Well-maintained inpatient rooms with round-the-clock care for antenatal, postnatal, gynecological, and surgical admissions.
On-site pharmacy stocking pregnancy-safe medications, supplements, iron, folic acid, and emergency drugs for maternal and newborn care.
Immediate access to stored blood and diagnostic labs supports timely interventions during obstetric emergencies and surgeries.
Collaborative care with pediatrics department ensures smooth transition from maternity to child health including immunization and growth monitoring.
Pamphlets, posters, and flipbooks to educate women on pregnancy diet, hygiene, newborn care, and family planning practices.
Skilled nursing and midwifery staff trained in labor support, neonatal care, breastfeeding guidance, and postnatal monitoring.
Clean, ventilated space with seating for patients and attendants waiting for eye consultation or treatment.
Linkage to main OT complex for complex surgeries requiring general anesthesia or multidisciplinary team involvement.
Quick-access water source for flushing eyes in case of chemical exposure, injury, or irritants.
Skilled support staff trained in vision testing, assisting procedures, and managing patient flow in the eye unit.
Referral network with tertiary hospitals for retinal, corneal, and pediatric surgeries requiring specialized equipment or expertise.
Pamphlets, posters, and leaflets used for school screening, community education, and program awareness under NPCB.
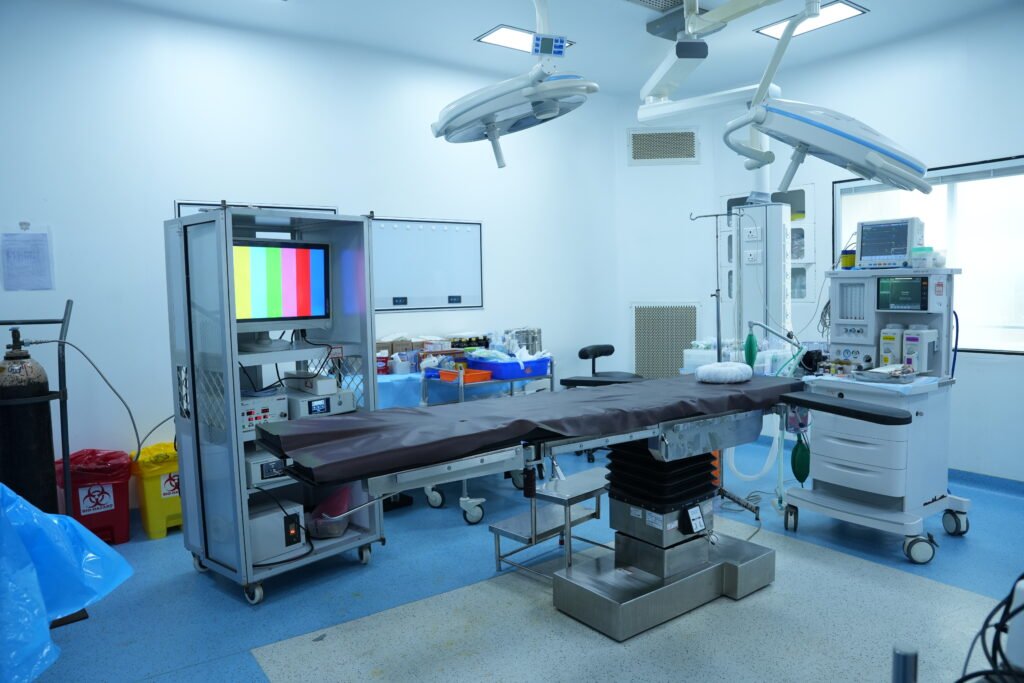
Advanced sterile surgical suite with modern ventilation and orthopedic-compatible equipment for performing both minor and major bone surgeries.
Specialized room for applying, adjusting, and removing orthopedic casts, braces, and splints in a sterile environment.
Seamless coordination for immediate orthopedic trauma response, ensuring quick transfer and care of fracture and injury cases.
Seamless connectivity to diagnostic and pharmacy services ensures timely investigations and availability of child-appropriate medication.
Pamphlets, charts, and posters offering guidance on childhood illnesses, feeding, immunization, and hygiene practices for parental awareness.
Dedicated area for one-on-one interaction between caregivers and nutrition counselors, often equipped with visuals and diet plans.
Area with ramps, bars, and aids designed to help patients regain walking ability and balance after limb loss or surgery.
On-site center equipped to design, fabricate, and customize prosthetic limbs, improving turnaround time and patient mobility outcomes.
Includes electrotherapy, heat/cold packs, and muscle stimulation tools for non-invasive, drug-free pain management.
Skilled professionals who craft, adjust, and train patients on prosthetic use, ensuring safe integration into daily life.
Patient-friendly space for accurate limb measurements and real-time fitting trials to ensure comfort, balance, and prosthesis usability.
Private area where patients and families receive lifestyle, mental health, and device-use guidance during physical rehabilitation.
Essential resuscitation equipment like Ambu bags, oxygen, and suction units to manage postpartum or neonatal emergencies immediately.
Private, calm space for lactation support, one-on-one counseling, and education on proper breastfeeding techniques.

Thermal cradles and monitoring devices to maintain newborn temperature, check vital signs, and detect early signs of distress.
Regular sanitation, disinfection routines, and secured access ensure patient safety, infection control, and family peace of mind.
Round-the-clock consultation and referral access to pediatricians and obstetricians for managing complications and providing expert postpartum care.
Trained nursing staff available at all hours to monitor recovery, assist in care, and provide emotional and clinical support.
Uninterrupted power supply systems protecting sensitive imaging equipment during electrical outages, ensuring continuous diagnostic services.
Personal dosimeters for radiology staff to monitor and record cumulative radiation exposure, ensuring occupational safety compliance.
Designated space for developing and storing radiographic films securely, applicable where analog radiology systems are used.
Dedicated private space for obtaining informed consent and providing counseling before sensitive imaging procedures like mammography or pelvic ultrasound.
Seamless coordination of radiology services across outpatient, inpatient, and emergency departments for efficient diagnostic support.
Skilled personnel managing radiology equipment, assisting with procedures, and supporting patient care under professional supervision.
System for scheduling general surgery cases, managing operation theatre logistics, and tracking surgical equipment usage.
Controlled access routes for staff, patients, and materials to maintain sterile conditions in the general surgery operation area.
Dedicated section for cleaning and disinfecting general surgery instruments as per hospital hygiene and safety protocols.
Area where post-surgical patients receive initial rehabilitation instructions, wound care guidance, and mobility support.
Private space for discussing surgical procedures, obtaining consent, and providing pre- and post-operative patient education.
Coordination between general surgery and emergency services ensuring timely surgical interventions during trauma and acute cases.
Digital platform managing patient records, reports, and scheduling for streamlined urology department operations and data security.
Controlled, hygienic spaces dedicated to cleaning, sterilizing, and storing urology-specific surgical and diagnostic instruments.
Procedure room for minor urological interventions under sterile conditions without requiring a full operating theatre setup.
Private space where patients receive pre- and post-procedure counseling, treatment education, and family support related to urological care.
Setup allowing same-day admission, procedure, and discharge for minor urological surgeries, ensuring convenience and quicker recovery.
Essential lab devices for preserving biological samples and separating blood components for analysis .
Designated laboratory areas to prevent cross-contamination and maintain sterile testing environments for different specializations.
Temperature-controlled unit used to safely store blood and plasma components for testing and transfusion readiness.
Computerized system for fast, secure, and paperless delivery of test results to physicians and patients.
Qualified professionals responsible for performing tests, handling samples, entering data, and ensuring result accuracy.
Structured process for sending specialized samples to NABL-accredited labs when tests aren’t available in-house.
Essential first-aid and emergency response tools available on-site to handle rare adverse reactions during cosmetic treatments.
Proper biomedical waste disposal system specifically for dermatology and cosmetology waste, ensuring compliance with health and safety standards.
Organized, hygienic storage cabinets for creams, serums, and procedural products, ensuring easy access and preservation of product quality.
Structured collaboration with dermatology specialists to ensure medical oversight for cosmetology treatments and handle any medical concerns.
Qualified staff assisting cosmetology professionals with procedures, patient care, and maintaining clinical hygiene and procedural efficiency.
Printed charts and displays showcasing expected treatment outcomes, helping patients set realistic expectations through visual guidance.
Comfortable and ventilated seating area with proper signage, water, and educational posters for patients awaiting consultation or treatment.
Color-coded bins and sharps disposal systems following biomedical waste regulations for safe and eco-friendly clinical waste disposal.
Designated shelves and storage units for organized, hygienic, and efficient management of dental materials and consumables.
Qualified support staff trained to assist dentists in procedures, sterilization, patient preparation, and clinical coordination.
Child-sized dental instruments and accessories designed for safe, comfortable treatment of young patients with minimal discomfort.
Standardized registers and formats used for reporting under the National Oral Health Programme, including outreach and treatment statistics.
Separate area near OPD/emergency where patients are assessed based on severity to prioritize treatment accordingly.
Visual aids and leaflets displayed in OPDs and wards to educate patients about diseases, prevention, and healthy practices.
Readily available fluids and essential emergency drugs like antipyretics, antibiotics, and cardiac stimulants for immediate intervention.
Qualified personnel trained in general medicine protocols, patient care, emergency response, documentation, and communication.
Seamless coordination with specialists for timely referral of complex cardiac, neurological, or endocrine cases requiring advanced care .
Spacious, ventilated seating areas with drinking water, display boards, and announcements for comfortable patient flow and reduced anxiety.
Collaboration with IDSP/NICD for timely reporting of infectious diseases and contribution to national health surveillance efforts.
Structured process for regularly verifying test accuracy, reagent reliability, and laboratory performance through controls and documentation.
Handouts, posters, and presentations used to train hospital staff on specimen collection, infection control, and antimicrobial stewardship.
Comfortable, discreet waiting area designed to respect patient confidentiality and reduce stress before consultations or therapy.
Formal partnerships with government and non-government organizations providing rehabilitation, social support, and post-treatment integration services.
Established protocols and documentation for referring patients to inpatient psychiatric facilities when intensive care is required.
Visually engaging posters displayed in clinic spaces to promote mental health awareness and encourage help-seeking behavior.
Available brochures, leaflets, and visual aids educating patients and families about mental health conditions, treatments, and wellness strategies.
A welcoming, stigma-free setting designed to promote mental well-being, safety, and comfort for all individuals seeking psychiatric care.
Uninterrupted power support system (e.g., generator, UPS) to maintain refrigeration and safety during outages.
Specific area for issuing blood and components with record-keeping and dispatch verification systems.
Restricted-access storage ensuring proper cold chain management and compliance with safety protocols during blood handling.
Qualified personnel responsible for donor screening, component processing, testing, and ensuring regulatory compliance.
Protective gear and proper biomedical waste bins to ensure safety and hygiene for staff and donors.
Display area showcasing donor appreciation, DHS certifications, and quality acknowledgments to promote transparency and morale.
Digital system to store, retrieve, and share MRI/CT scans securely across departments, enhancing neuroimaging-based decisions.
Dedicated network to quickly retrieve and review large neuroimaging files for diagnosis and cross-department consultation.
Outpatient chambers equipped with neuro reflex hammers, fundoscopy tools, tuning forks, BP monitors, and neurological charts.
Virtual consultation platform for neurology patients in remote areas, including follow-up care, screening, or second opinions via video.
Referral access to pathology and radiology for blood tests, biopsies, scans, and histopathological confirmation of cancer.
Standard PPE kits and color-coded bins ensure infection control and safe biomedical waste disposal during chemo and procedures.
Educational charts, posters, and banners used in OPD or camps to spread awareness on early symptoms and prevention.
Dedicated contact point to facilitate referrals, feedback, reporting, and coordination with district/state oncology programs and cancer control initiatives.
Structured digital/physical record system for tracking cancer screenings, diagnosis, treatment status, and reporting under the NCD program.
Logistical help and formal referral coordination for cancer patients needing surgery, radiotherapy, or advanced care at regional centers.